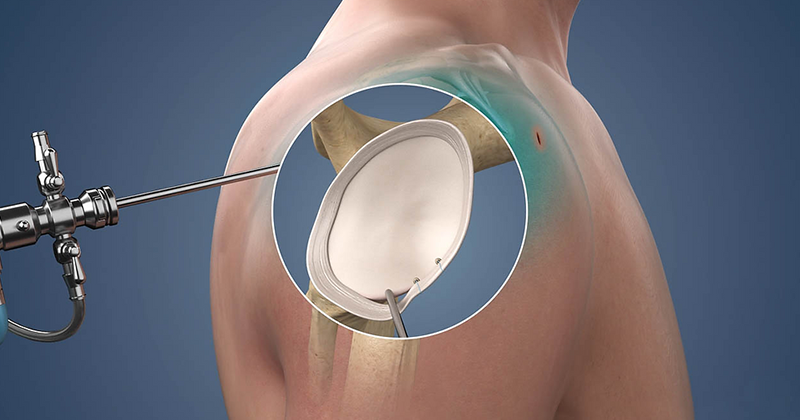
Arthroscopic Bankart surgery
Shoulder dislocations, particularly anterior dislocations, can lead to a Bankart lesion, which is a tear of the labrum—the cartilage ring that stabilizes the shoulder joint. This injury often results in recurrent dislocations, pain, and weakness. When conservative treatments such as physical therapy fail to prevent repeated instability, arthroscopic Bankart repair is indicated.
Arthroscopic Bankart repair is a minimally invasive procedure that uses an arthroscope—a small camera inserted through tiny incisions—to visualize and repair the torn labrum. During the procedure, the surgeon reattaches the labrum to the glenoid (shoulder socket) using sutures or anchors. This restores stability to the shoulder, prevents recurrent dislocations, and improves joint function. Compared to open surgery, arthroscopy offers smaller incisions, less soft tissue damage, reduced pain, and faster recovery.
The surgery is performed under general anesthesia, often with a regional nerve block to reduce postoperative pain. After the procedure, the shoulder is typically immobilized in a sling for several weeks to protect the repair. Early rehabilitation focuses on gentle range-of-motion exercises, gradually progressing to strengthening exercises for the rotator cuff and shoulder stabilizers. Full recovery may take 4–6 months, depending on the patient’s age, activity level, and adherence to rehabilitation protocols.
Complications are uncommon but may include infection, stiffness, recurrent instability, or nerve injury. Overall, arthroscopic Bankart repair is highly effective, with most patients regaining shoulder stability, reducing pain, and returning to daily, recreational, and athletic activities.
In summary, arthroscopic Bankart surgery provides a safe, minimally invasive solution for recurrent anterior shoulder instability. By repairing the labrum and restoring normal joint mechanics, it helps patients regain confidence, shoulder function, and quality of life.