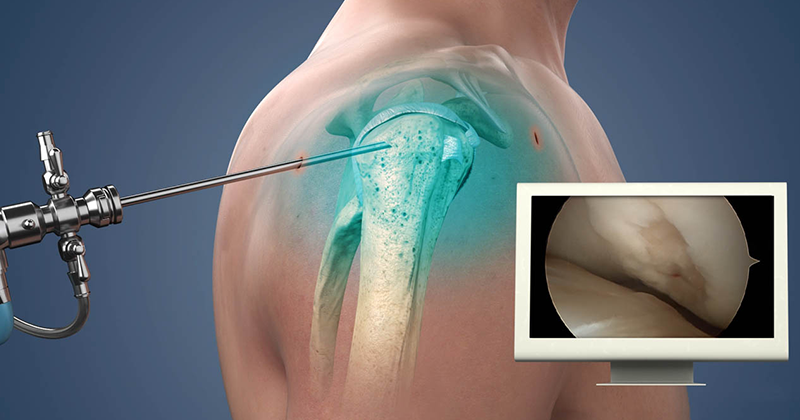
Arthroscopic Rotator cuff surgery
Rotator cuff tears are a common cause of shoulder pain, weakness, and limited range of motion. They can result from acute injuries, repetitive overhead activities, or degenerative changes with aging. When non-surgical treatments such as physical therapy, anti-inflammatory medications, and activity modification fail to relieve symptoms, arthroscopic rotator cuff repair may be indicated.
Arthroscopic surgery is a minimally invasive technique that uses a small camera (arthroscope) and specialized instruments inserted through tiny incisions around the shoulder. This approach allows the surgeon to visualize the torn tendons, remove inflamed tissue or bone spurs, and reattach the torn rotator cuff tendon to the humeral head using sutures or anchors. Compared to traditional open surgery, arthroscopy results in smaller scars, less soft tissue trauma, reduced postoperative pain, and faster recovery.
The procedure is usually performed under general anesthesia, sometimes combined with a regional nerve block for pain control. Postoperatively, the shoulder is immobilized in a sling for several weeks to protect the repair. Early rehabilitation focuses on gentle passive movements, gradually progressing to active exercises and strengthening under the guidance of a physical therapist. Recovery may take 4–6 months, depending on tear size, tendon quality, and patient compliance with rehabilitation.
Complications are uncommon but can include infection, stiffness, re-tear of the tendon, or nerve injury. Success rates are generally high, with most patients experiencing significant pain relief, improved shoulder function, and enhanced quality of life.
Overall, arthroscopic rotator cuff surgery is a safe and effective procedure for patients with persistent shoulder pain or functional limitations due to rotator cuff tears. By combining precise surgical repair with structured rehabilitation, patients can regain shoulder strength, mobility, and the ability to perform daily and recreational activities.